NOTE: This article is the second in a series of 10 articles and is part of our Economic Evaluation in Healthcare 101 course. You can find a course overview and links to all 10 course modules here:
- Economic Evaluation in Healthcare 101: Course Overview
- Introduction to Economic Evaluation in Healthcare
- Types of Economic Evaluation in Healthcare
- Measuring Costs in Healthcare
- Measuring Health Outcomes
- Decision Analytic Modeling in Economic Evaluation
- Data Sources for Economic Evaluation in Healthcare
- Interpreting and Applying Economic Evaluation Results in Healthcare
- Economic Evaluation in Health Technology Assessment (HTA)
- Ethical and Equity Considerations in Economic Evaluation
- Future Trends in Economic Evaluation in Healthcare
Types of Economic Evaluations in Healthcare
Healthcare systems around the world face the dual challenge of rising costs and finite resources. Economic evaluation plays a critical role in helping decision-makers allocate those resources efficiently by assessing the value for money of competing healthcare interventions. Among the various forms of economic evaluation, five key approaches stand out: Budget Impact Analysis (BIA), Cost-Minimization Analysis (CMA), Cost-Effectiveness Analysis (CEA), Cost-Utility Analysis (CUA), and Cost-Benefit Analysis (CBA). Each method serves distinct purposes and is suited to specific decision-making contexts.
1. Budget Impact Analysis (BIA): Financial Feasibility in Real-World Settings
Budget Impact Analysis estimates the financial consequences of adopting a new healthcare intervention within a specific setting and timeframe, typically a payer’s annual or multi-year budget window.
When and how to use it:
- BIA is often conducted alongside cost-effectiveness analysis during health technology assessments (HTAs), especially when a new treatment is being considered for inclusion in a reimbursement list or formulary.
- It considers variables such as eligible population size, uptake rates, substitution effects, and drug acquisition costs.
- It typically focuses on short-term affordability, not long-term value.
Key differences with other evaluations:
- Unlike CEA or CUA, BIA does not compare health outcomes but rather models the impact on the payer’s budget.
- While CEA asks, “Is it worth it?”, BIA asks, “Can we afford it?”
Reference: Sullivan SD et al. (2014). Budget impact analysis—principles of good practice. Value in Health, 17(1), 5–14.
2. Cost-Minimization Analysis (CMA): Focus on Least-Cost Option When Outcomes Are Equal
Cost-Minimization Analysis is a simplified form of economic evaluation used only when clinical outcomes of competing interventions are proven to be equivalent.
When and how to use it:
- CMA is appropriate when interventions have identical effectiveness and safety profiles (e.g., a generic vs. branded drug).
- The analysis focuses solely on comparing costs, including acquisition, administration, and monitoring.
Limitations:
- CMA requires rigorous evidence of equivalence, which is rarely available outside of bioequivalent drug comparisons.
- Misapplication of CMA without proven equivalence may lead to misleading conclusions.
Reference: Drummond MF et al. (2015). Methods for the Economic Evaluation of Health Care Programmes (4th ed.). Oxford University Press.
3. Cost-Effectiveness Analysis (CEA): Comparing Costs per Health Outcome
Cost-Effectiveness Analysis evaluates the cost per unit of health outcome—such as life-years gained, strokes prevented, or infections avoided.
When and how to use it:
- CEA is useful when outcomes are measured in natural units and can be compared across similar interventions.
- It produces an Incremental Cost-Effectiveness Ratio (ICER), calculated as:
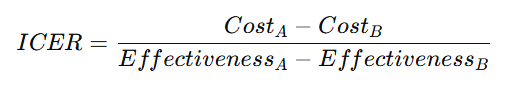
Example:
- If Treatment A costs $50,000 and yields 5 life-years, and Treatment B costs $30,000 for 4 life-years, the ICER is $20,000 per life-year gained.
Limitations:
- CEAs are not well-suited for comparing across diseases (e.g., mental health vs. cancer), as outcomes are not standardized.
Reference: Neumann PJ et al. (2016). Cost-Effectiveness in Health and Medicine, 2nd ed.
4. Cost-Utility Analysis (CUA): Quality and Quantity of Life in a Single Metric
Cost-Utility Analysis extends CEA by incorporating quality of life, using standardized metrics such as Quality-Adjusted Life Years (QALYs) and Disability-Adjusted Life Years (DALYs).
- QALYs combine survival and health-related quality of life on a scale from 0 (death) to 1 (perfect health).
- DALYs reflect years lost to illness, disability, or premature death—commonly used in global health settings.
When and how to use it:
- CUA is most appropriate when both longevity and quality of life are affected.
- It allows for comparisons across diseases and interventions, enabling resource allocation at a population level.
Policy relevance:
- Many agencies, like NICE in the UK, use cost per QALY thresholds (e.g., £20,000–30,000/QALY) to determine funding eligibility.
Example:
- A new drug provides 1.5 additional QALYs at an incremental cost of $45,000 → cost per QALY = $30,000.
Reference: Weinstein MC et al. (1996). Recommendations of the Panel on Cost-Effectiveness in Health and Medicine. JAMA, 276(15), 1253–1258.
5. Cost-Benefit Analysis (CBA): Monetizing Both Costs and Benefits
Cost-Benefit Analysis expresses both costs and benefits in monetary terms, allowing direct comparison across sectors (e.g., healthcare vs. education).
The key metric in CBA is the Net Benefit (NB):
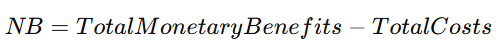
When and how to use it:
- CBA is useful for broad policy decisions, such as evaluating public health programs or regulatory interventions.
- Benefits are often estimated using willingness to pay (WTP) or human capital methods to assign monetary value to outcomes like life-years saved or improved productivity.
Advantages:
- Facilitates intersectoral comparisons and prioritization across government programs.
- Helps estimate net monetary benefit: if benefits exceed costs, the intervention is worth implementing.
Challenges:
- Assigning monetary value to life, pain, or dignity raises ethical and methodological issues.
- Estimations can vary widely depending on assumptions and population context.
Reference: Boardman AE et al. (2018). Cost-Benefit Analysis: Concepts and Practice (5th ed.). Cambridge University Press.
Conclusion
Understanding the various types of economic evaluation is fundamental to evidence-informed healthcare policy. Each method—whether it prioritizes budget impact, clinical equivalence, natural health outcomes, utility measures, or monetized benefits—serves a distinct purpose. Together, they provide a toolkit for balancing economic feasibility, ethical fairness, and clinical value in the design and delivery of health services.
References
- Drummond MF, Sculpher MJ, Claxton K, Stoddart GL, Torrance GW. (2015). Methods for the Economic Evaluation of Health Care Programmes, 4th ed. Oxford University Press.
- Sullivan SD, Mauskopf JA, Augustovski F, et al. (2014). Budget impact analysis—principles of good practice. Value in Health, 17(1), 5–14.
- Neumann PJ, Sanders GD, Russell LB, Siegel JE, Ganiats TG. (2016). Cost-Effectiveness in Health and Medicine, 2nd ed. Oxford University Press.
- Weinstein MC, Siegel JE, Gold MR, et al. (1996). Recommendations of the Panel on Cost-Effectiveness in Health and Medicine. JAMA, 276(15), 1253–1258.
- Boardman AE, Greenberg DH, Vining AR, Weimer DL. (2018). Cost-Benefit Analysis: Concepts and Practice, 5th ed. Cambridge University Press.
